In December 2016, two Naval aviators in an EA-18G Growler suffered catastrophic injuries after their cockpit pressure system malfunctioned, causing an explosive decompression.
The aviators, assigned to Naval Air Station Whidbey Island, Washington, were rushed to a nearby medical center.
One of them was not breathing, requiring CPR and a tube to support his airway. He sustained a severe brain injury and facial fractures. The other crew member suffered from rapidly deteriorating lung issues that required a needle decompression to release built-up pressure.
The two aviators likely would have died that day without the critical advanced life support skills of the two Navy search and rescue medical technicians, or SMTs, who cared for them en route to the hospital, according to documents obtained by Marine Corps Times.
But those two SMT medics were the only ones at the naval air station who had national-level paramedic certification, giving them the skills needed to keep the two aviators alive.
The Navy has a severe shortage of flight medics. And the medics it does have rarely earn the paramedic qualifications that are required by the Army, Air Force and the civilian world.
The Navy and Marine Corps are the only DoD branches that do not provide paramedic certification to flight medics during their training pipeline. Astonishingly, those who do earn those certifications — like those responding to the Whidbey Island incident — pay for it out of their own pocket and get it on their own time.
The SMTs are the medics that are responsible for the Navy’s search and rescue mission and at times whisking Marines off the battlefield, ensuring they stay alive until they reach a full-scale medical facility for surgery and other lifesaving care.
Yet only six SMTs in the Navy are certified by the National Registry of Emergency Medical Technicians, Navy officials say. And the field is manned at only 54 percent, with only 80 medics in the fleet.
RELATED
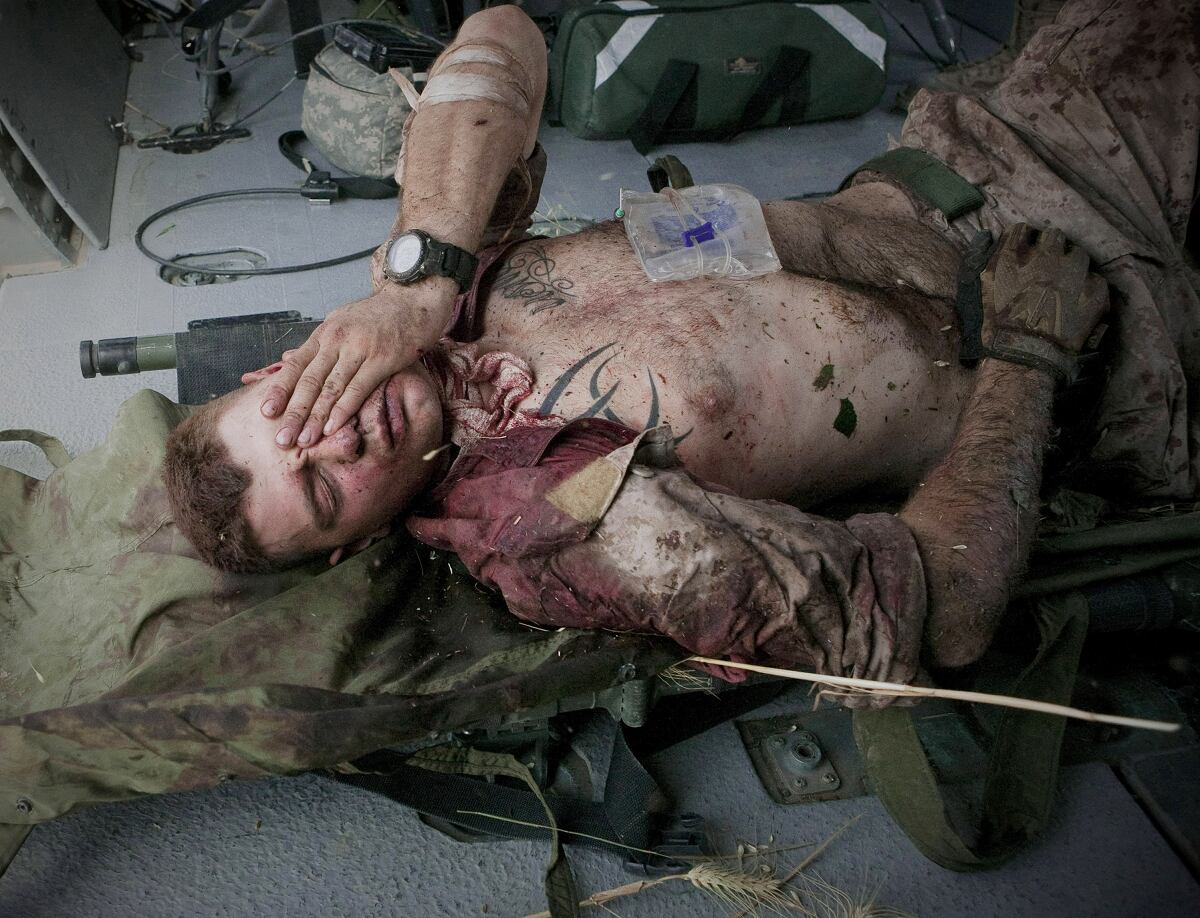
The two problems are linked, critics say, as flight medics are routinely leaving the field out of fear their inadequate training may result in the death of a patient.
“The SMT field is undermanned because they aren’t trained the right way,” a Navy official told Marine Corps Times on condition of anonymity. “They don’t want to be responsible for someone dying on them because they don’t have the right training and certifications.”
The lack of paramedic certification for Navy SMTs and Fleet Marine Force corpsman serving as casualty evacuation flight medics calls into question whether the services are fully prepared for a major war in which the force may not entirely control the battlespace.
“You’re looking at 18- to 19-hour long transports in a Pacific fight,” the Navy official said. “People could be stuck for a week, and now you’re talking about multiorgan failure, sepsis. These are the types of patients we are going to be seeing in the next battle.”

Right now, the Navy and Marine Corps do not have properly certified flight medics to care for these kinds of casualties.
That’s in part a reflection of the Navy’s training program, which emphasizes aircraft safety and familiarization, teaching future SMTs how to operate on aircraft like the Navy’s MH-60 helicopters.
Out of the nearly 18-month training pipeline for SMTs, only about seven weeks of training is geared toward emergency medicine.
It’s a source of frustration, and anger.
“The SMTs don’t need to go through months of training to learn about hydraulic fluid on a helicopter,” the Navy official said.
RECOMMENDATIONS IGNORED
The lack of training is a problem the Navy has known about for years, according to documents obtained by Marine Corps Times. Navy and Defense Department memos and letters going back years have recommended paramedic certification and training standardization for aeromedics involved in tactical combat casualty evacuations.
But the Navy has failed to impose any requirements for that level of training.
To make matters worse, if frears about major combat are realized, field and flight medics alike will need to be able to sustain and care for patients for longer durations of time than has been the recent custom.
The mature operating environments in Iraq and Afghanistan allowed wounded troops to be whisked off the battlefield within their first hour of injury. And those air ambulances were typically operated by Army and Air Force assets.
“The last 15 years of war, we pretty much adapted to the operational environment and dominated it,” Rear Adm. Colin G. Chinn, Joint Staff surgeon, said at a Navy medical symposium held at Marine Corps Base Quantico, Virginia, in February. “We are not going to have all the advantages we have now.”
In 2009, then-Defense Secretary Robert Gates implemented the “golden hour” policy, a promise by defense officials to surge medical assets to the conflicts in the Middle East to help speed up medical and casualty evacuations.
“But in a future fight that may not be the case,” Chinn said. “We need to be ready now.”
SMT training has been a concern among top Navy officials for years.
In 2015, the four-star admiral at Fleet Forces Command wrote a letter to the Navy’s surgeon general calling for paramedic certifications for SMTs.
The Navy’s SMTs are a “vital link” charged with “life sustaining care,” he wrote in the letter, a copy of which was obtained by Marine Corps Times, but “in times of conflict” those medics could confront trauma that was “beyond (their) level of training.”
Officials at the Bureau of Navy Medicine offered no explanation for the manning shortfall or the lack of paramedic certification for the Navy’s primary rotary wing search and rescue and casualty evacuation, or CASEVAC, units.
The Navy only said that officials are considering more advanced training for its hospital corpsman and SMT medics to prepare for this future fight. BUMED officials offered few details.
“We developed and implemented the Hospital Corpsman Personnel Qualification Standard, and are partnering with John H. Stroger Jr. Hospital of Cook County in Illinois to test a concept in which hospital corpsmen receive hands-on trauma training at civilian facilities,” Navy spokesman Charles Gulick told Marine Corps Times.

“Additionally, we are exploring opportunities to recruit personnel directly into the SMT pipeline and researching possibilities for more advanced medical training.”
But that training applies to sailors stationed at Navy Medicine treatment facilities, headed for assignments where they will work at medical facilities aboard ships or submarines.
The Navy’s training efforts focus more heavily on the clinical hospital corpsmen at larger facilities rather than the field and flight medics who operate at the front lines of battle.
These folks “work in a controlled environment that’s not mobile, in a facility with nurses, doctors, physician assistants, practitioners under the control of competent medical professionals,” the Navy official argued.
“We work in the back of a helicopter, at night, both in the Navy and Marine Corps, and we don’t have any certification,” he added.
Gulick says the Navy is looking at options to provide hospital corpsmen with hands-on training. One example is an initiative to put them “at alternative sites outside the typical shore hospital or clinic providing non-urgent, walk-in medical care.”
Marines wounded in combat in Iraq have, at times, been medevaced off the battlefield by SMT medics serving with the 2515th Naval Air Ambulance Detachment. The 2515th transported more than 2,000 patients during its tenure in Iraq, but was disbanded several years ago.
Since then, the Corps has sought to step up its own training of flight medics, sending its Fleet Marine Force corpsmen through a hodgepodge of training that generally mirrors that of the SMTs, but still has no paramedic certification.
It’s not a standardized pipeline and doesn’t have its own military occupational specialty, Marine Corps Times has learned.
The Navy and Marine Corps may be headed for troubled waters.
Accustomed to Air Force and Army medevac and casevac for the past 17 years in Iraq and Afghanistan, with paramedic certified flight medics, the Corps and the Navy are now playing catch up to prepare for a possible fight in the Pacific, where Army and Air Force assets may not be available to whisk sailors and Marines to higher level treatment facilities.
“If I had an E-3 sailor or Marine drive to work in the morning and she crashed her car and had horrific injuries — amputation, fracture or collapsed lung — and the trauma center was 45 minutes away, a paramedic would be transporting her, providing advanced life support care,” the Navy official said.
TRAINING DEFICIENCY
Documents show the Navy has debated the need for paramedic training for more than 20 years.
In 1995, the Navy attempted to gain seats at the Air Force’s Pararescue, or PJ, school to help Navy flight medics earn paramedic certification. But those efforts came to a halt over cost concerns and the expected closure of the PJ school at Kirtland Air Force Base in Albuquerque, New Mexico, documents show.
In 2011, the Tactical Combat Casualty Group with the Defense Health Board, known as the TCCC, recommended that tactical casualty evacuation platforms be “staffed with in-flight care providers to meet or exceed the civilian standard.”
The working group stated that critical care flight transports should include at least two of the following and one of the following per “critical casualty”: critical care flight trained paramedic, critical care flight trained nurse, critical care flight trained physician, critical care flight trained certified nurse practitioners or physician assistants.
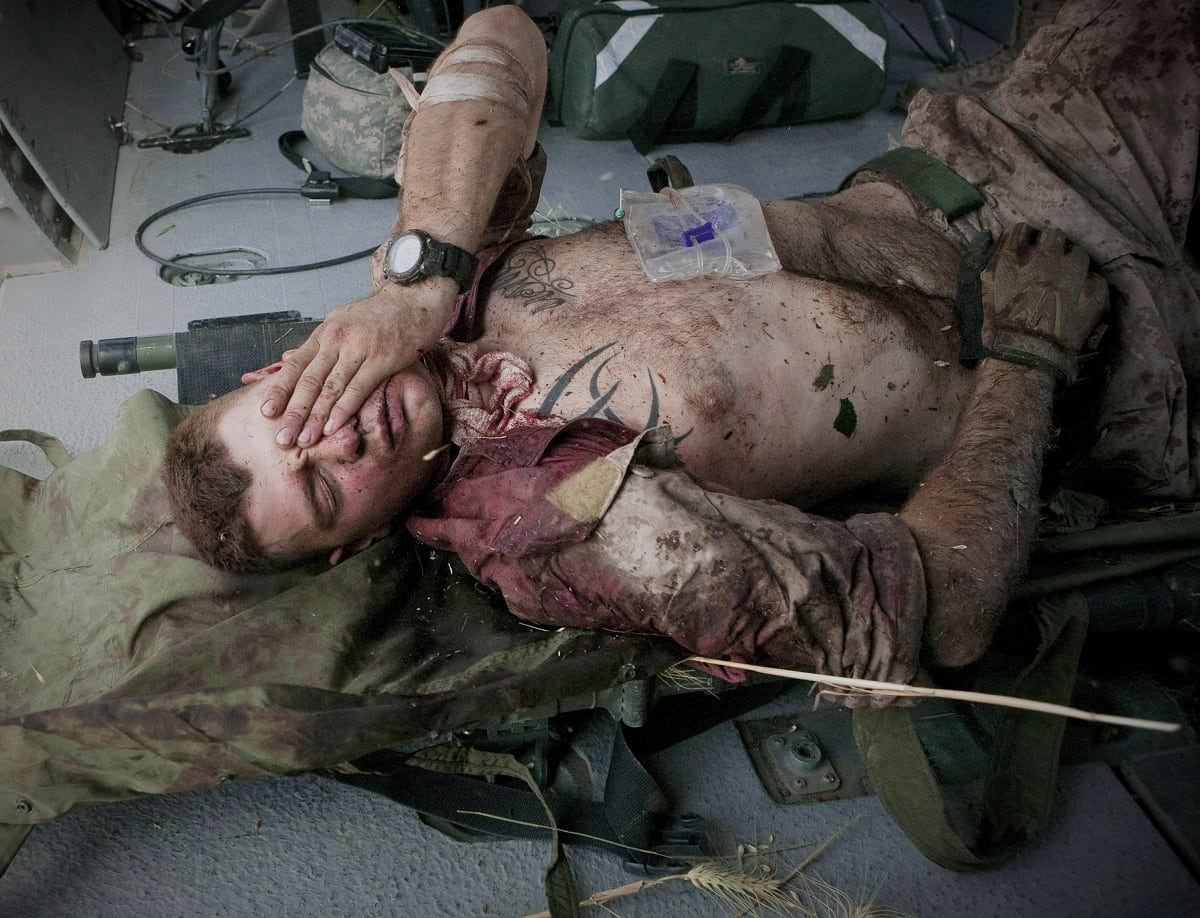
“Combat trauma deaths occur for the most part in the pre-hospital phase of care, highlighting the need to optimize care during this period,” the TCCC working group said in an August 2011 review. “Advanced provider skill level (above EMT-B level) during transport of the severely wounded improves survival.”
A March 2015 study of combat trauma lessons learned from the Defense Health Board also called for the DoD to harmonize training of tactical casualty evacuation medics across the services at one high standard. That standard was the 160th Special Operations Aviation Regiment (Airborne), Air Force Special Operations Command, or the Amy Medical Department model. All these models include nationally accredited paramedic certification.
Furthermore, the Joint Requirements Oversight Council endorsed the findings of the TCCC working group in a 2012 memo, obtained by Marine Corps Times. The JROC is chaired by the vice chairman of the Joint Chiefs of Staff and makes recommendations to the DoD.
The JROC memo called for the services to implement actions as “outlined in the enclosure.” That enclosure called for the services to review training for their enlisted flight medics who may serve in tactical environments against the flight paramedic certified, or FP-C, level accreditation and to develop a plan to certify and sustain it by fiscal 2016.
Following that review the Navy recommended paramedic certification for its SMT medics in a series of correspondence dated April 26, 2013; Aug. 3, 2015; Aug. 24, 2015; and Nov. 9 2015.
“Currently the U.S. Air Force and the U.S. Army provide paramedic level training for their Medical Technicians that support SAR and evacuation missions,” stated an April 26, 2013, letter from the commander of Naval Air Forces Pacific to the chief of the Bureau of Medicine and Surgery. “In contrast, the Navy SMTs receive only Basic Emergency Medical Training that is augmented with three advanced lifesaving courses.”
The letter outlined that the training did not meet requirements to support special operations forces missions that Naval Air Pacific was being tasked to support.
“As has been done in other services, a Navy paramedic training program for SMTs must be implemented immediately,” the April letter states.
“To better support the Fleet, all Search and Rescue Medical Technicians (SMT/HM-8401) must be National Registry of Emergency Medical Technicians-Emergency Medical Technician Paramedic certified, and Flight Paramedic Certified,” stated an Aug. 3, 2015, letter from Naval Air Forces Pacific to the surgeon general of the Navy. “This training requirement brings the U.S. Navy in alignment with other Department of Defense, Interagency, and civilian aeromedical evacuation standards.”
A correspondence from the commander of U.S. Fleet Forces Command to the surgeon general of the Navy, dated Nov. 9, 2015, further called for paramedic certification for SMT medics.
LAGGING BEHIND
So what is everyone else up to?
Air Force Pararescue has incorporated paramedic certification for its medics since 1995. Army DUSTOFF medics were mandated by Congress in 2012 to have paramedic certification.
Air Force PJs undergo rigorous emergency medicine training that includes nearly 45 weeks of advanced medical training, said Lt. Col. Michael Sumner, the deputy command surgeon for U.S. Special Operations Command.
Medics with the 160th SOAR attend nearly 18 months of training that includes the Special Operations Combat Medic Course and the Special Operations Aviation Medical Indoctrination Course, which lasts approximately 10 weeks.
RELATED

Fully mission-qualified medics with 160th SOAR maintain two civilian certifications: National Registry Paramedic and Flight Paramedic–Certified, Maj. Harold A. Tate, a spokesman with U.S. Army Special Operations Aviation Command, told Marine Corps Times in an email.
Special operations medics with SOCOM go through a 36-week intensive medical training package called SOCOM-Advanced Tactical Paramedic, or SO-ATP that includes, EMT-paramedic-level skills in emergency cardiac care and emergency trauma care, advanced TCCC, TCCC instructor, tactical medical emergency management protocols, military medicine and preventive medicine,” Sumner said.
The Navy and Marine Corps’ flight medics are the only ones not getting paramedic certifications; this despite the fact that the SMT mission is to perform advanced life support independent of a medical officer during search and rescue, casualty evacuation or medevac missions.
The Navy claims advanced training is in the works for its SMTs in the future but wouldn’t provide further details of what that training would entail.
In the meantime, the Navy says its current SMTs can achieve their paramedic certifications through an online portal called Navy Cool, which guides sailors through certifications related to their fields, Gulick told Marine Corps Times.
But if the poor manning numbers across the search and rescue medical technician community, and the handful of SMTs with the paramedic certification, are any kind of an indicator, it appears unlikely a large number of SMTs will be obtaining these necessary lifesaving skills anytime soon.
Shawn Snow is the senior reporter for Marine Corps Times and a Marine Corps veteran.





